In today's healthcare environment, understanding various medical technologies is crucial. One critical aspect is suction systems, often used in clinical settings. Dr. Jonathan Reynolds, a leading expert in respiratory care, eloquently notes, "The choice between open and closed suction systems can significantly impact patient outcomes." This statement highlights the importance of grasping the nuances involved in using these systems.
So, what is the difference between an open and closed suction system? Open systems require disconnection from ventilators, exposing patients to potential infections. Conversely, closed systems maintain ventilation during suctioning, minimizing risk. Each system has its unique benefits, yet the right choice can depend on specific clinical situations and patient needs.
These distinctions are not always clear-cut. Healthcare professionals must weigh factors like infection control and ease of use. A poorly chosen system might lead to complications. Thus, understanding these differences is vital for ensuring patient safety and comfort.
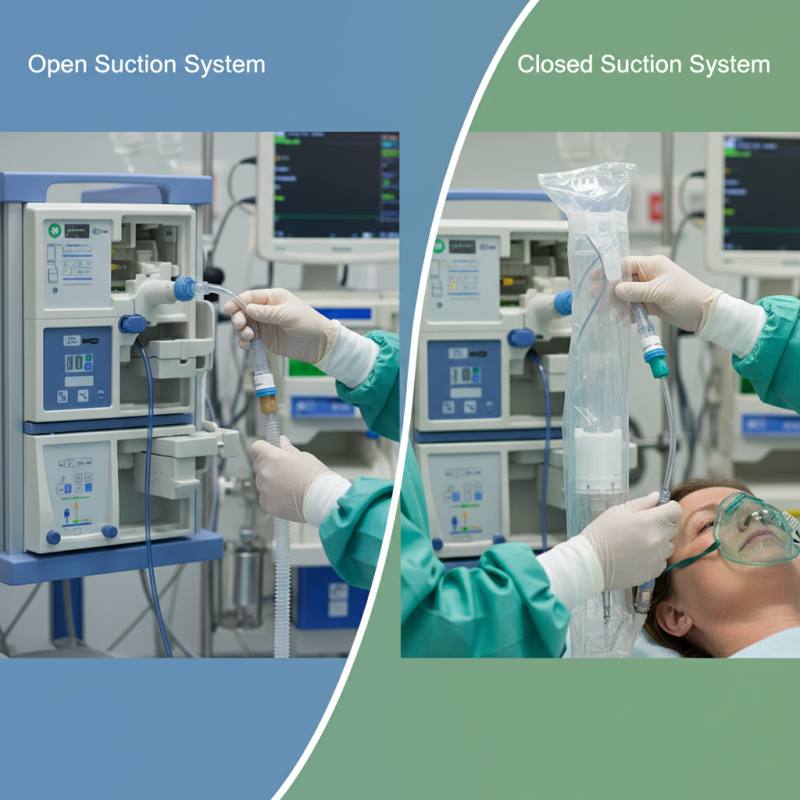
The choice between open and closed suction systems is critical in medical practice. Open systems rely on gravity to remove secretions, while closed systems use a tube within a protective sheath. This difference affects infection rates and patient comfort. According to a 2020 study published in the Journal of Hospital Infection, closed systems reduce ventilator-associated pneumonia (VAP) rates by up to 30%.
In practice, closed suction systems typically extend the duration of ventilation by allowing for safer suctioning without disconnecting from the ventilator. However, they can be more expensive, leading to budgetary concerns in healthcare settings. A report from the American Respiratory Care Foundation indicates that while initial costs are higher, the potential savings from reduced complications may justify the investment.
Despite these advantages, some healthcare professionals express concerns about the risk of occlusion in closed systems. Regular maintenance is crucial to prevent such issues. Training staff to effectively use both systems is vital. Understanding the strengths and weaknesses of each can help ensure optimal patient outcomes and resource management in diverse clinical environments.
Open suction systems play a vital role in patient care, offering several advantages over their closed counterparts. One key benefit is enhanced accessibility. Healthcare providers can quickly clear airway obstructions using open systems. This immediacy makes a significant difference in emergency situations where every second counts. The ability to manually regulate suction levels allows clinicians to tailor their approach based on individual patient needs.
However, open systems also come with some disadvantages. The risk of infection is higher since these systems are exposed to the air. Moreover, the requirement for regular cleaning and maintenance adds to their operational complexity. Clinicians must be vigilant in managing these challenges to ensure patient safety.
Tips for using open suction systems effectively include regularly training staff on proper techniques. This promotes consistency and reduces the potential for error. Additionally, standardizing protocols for cleaning can mitigate infection risks. Keep suction equipment organized and accessible to streamline the process during critical moments. While open suction systems offer distinct advantages, they are not without their challenges, requiring ongoing reflection and adaptation in clinical practice.
Closed suction systems are designed to enhance safety and efficiency during suction procedures. These systems typically use a sealed mechanism, allowing for continuous suction without exposing patients to open air. This feature reduces the risk of infection and ensures a sterile environment. Medical professionals often appreciate this benefit, making these systems a preferred choice in many clinical settings.
Tips: Always check the integrity of the closed system before use. A small breach can compromise sterility.
Another key advantage of closed suction systems is their ability to function without interrupting the ventilatory support. This allows for frequent assessments of the airway without causing distress to the patient. Operators can perform suctioning quickly and effectively, maintaining patient comfort. However, staff training is crucial to ensure that all procedures are performed correctly. Lack of awareness can lead to mistakes that may derail the benefits of the system.
Tips: Regular training and refresher courses can improve staff competence. Always encourage team discussions about challenges faced during suctioning operations.
This chart illustrates the comparison between Open and Closed Suction Systems based on effectiveness, infection risk, ease of use, cost-effectiveness, and patient comfort. Each category provides insight into the strengths and weaknesses of both systems in clinical settings.
Open and closed suction systems serve distinct needs in clinical settings.
Open systems allow suctioning directly into the environment, exposing healthcare workers and patients to potential contaminants.
These systems can be effective but may lead to cross-contamination and increased infection risks.
On the other hand, closed suction systems encase the suction catheter.
This design minimizes exposure and reduces the risk of infection.
Studies show that closed systems result in fewer pulmonary infections and are less stressful for patients.
The ease of use contributes to quicker procedures, but they might require more training for proper application.
Evaluating clinical outcomes is crucial.
While open systems may be more familiar to some staff, the benefits of closed systems can be significant.
Research indicates that closed systems often yield better recovery results, highlighting the need for facilities to reflect on their suctioning techniques.
Adopting the best method can directly impact patient safety and recovery.
In suction system use, safety is paramount. Understanding the differences between open and closed suction systems helps mitigate risks. Open systems expose patients to more environmental factors. This can lead to higher infection rates. In contrast, closed systems offer a barrier that reduces pathogen exposure. Proper training for healthcare professionals is essential to maximize safety.
Infection control measures often include regular equipment sterilization and proper disposal techniques. Even experienced professionals can overlook the importance of these steps. Routine audits can identify gaps in practices. Moreover, maintaining a clean environment during suction procedures is critical. This ensures that the risk of cross-contamination is minimized.
Communication among healthcare staff plays a vital role. It enhances awareness of potential hazards and promotes adherence to safety protocols. Frequent discussions about infection risks can keep everyone vigilant. Education about best practices can also help reduce complacency. Such strategies contribute to safer patient outcomes.
: Open systems rely on gravity, while closed systems use a tube in a sheath. This affects infection rates and patient comfort.
Closed systems can reduce VAP rates by up to 30%, making them safer for patients on ventilators.
Closed systems are often more expensive initially. Budgetary concerns can limit their adoption in some settings.
Open systems offer quick access to airway obstructions, making them effective in emergencies when time is crucial.
They have a higher infection risk due to air exposure and require diligent cleaning and maintenance.
Regular training on techniques and standardizing cleaning protocols can promote safety and reduce errors.
Check the integrity of the system before use. A breach can compromise sterility and patient safety.
Proper training ensures correct procedures, enhancing benefits. Ongoing reflection on challenges faced is essential.
Understand each system's strengths and weaknesses to ensure optimal patient outcomes and proper resource management.
Continuous reflection can help healthcare providers adapt practices to improve patient care and safety outcomes.
The article explores the question, "What is the difference between an open and closed suction system?" in medical practice, highlighting the comparative aspects and clinical implications of each system. Open suction systems offer advantages such as straightforward application and effectiveness in specific scenarios, making them beneficial for patient care in certain settings. In contrast, closed suction systems are characterized by their key features and operational mechanisms designed to minimize infection risks and enhance patient safety.
When assessing clinical outcomes, the efficacy of open versus closed suction techniques reveals important distinctions in their performance and suitability for various clinical conditions. Safety considerations and infection control practices further underscore the need for healthcare professionals to be aware of the implications of each system, reinforcing their importance in effective patient management.

 Mainline Medical
Mainline Medical